Partial Sacralization Left L5 Segment Is Again Appreciate
Enquiry Article Articles
A Review of Symptomatic Lumbosacral Transitional Vertebrae: Bertolotti'south Syndrome
International Journal of Spine Surgery January 2015, 9 42; DOI: https://doi.org/10.14444/2042

Abstract
Background Lumbosacral transitional vertebrae (LSTV) are increasingly recognized as a common anatomical variant associated with contradistinct patterns of degenerative spine changes. This review will focus on the clinical significance of LSTV, disruptions in normal spine biomechanics, imaging techniques, diagnosis, and treatment.
Methods A Pubmed search using the specific key words "LSTV," "lumbosacral transitional vertebrae," and "Bertolotti'due south Syndrome" was performed. The resulting group of manuscripts from our search was evaluated.
Results LSTV are associated with alterations in biomechanics and anatomy of spinal and paraspinal structures, which have important implications on surgical approaches and techniques. LSTV are oft inaccurately detected and classified on standard AP radiographs and MRI. The employ of whole-spine images too equally geometric relationships between the sacrum and lumbar vertebra increment accurateness. Uncertainty regarding the crusade, clinical significance, and treatment of LSTV persists. Some authors suggest an association between LSTV types II and 4 and low back pain. Pseudoarticulation between the transverse process and the sacrum creates a "false joint" susceptible to arthritic changes and osteophyte formation potentially leading to nerve root entrapment.
The diagnosis of symptomatic LSTV is considered with advisable patient history, imaging studies, and diagnostic injections. A positive radionuclide study along with a positive effect from a local injection helps distinguish the transitional vertebra every bit a significant hurting source. Surgical resection is reserved for a subgroup of LSTV patients who fail conservative handling and whose pain is definitively attributed to the anomalous pseudoarticulation.
Conclusions Due to the common finding of low back hurting and the wide prevalence of LSTV in the general population, it is essential to differentiate between symptoms originating from an anomalous psuedoarticulation from other potential sources of low back pain. Further studies with larger sample sizes and longer follow-up fourth dimension would better demonstrate the effectiveness of surgical resection and assist guide treatment.
- LSTV
- Bertolotti'southward Syndrome
- transitional vertebrae
Introduction
Lumbosacral transitional vertebrae (LSTV) are congenital spinal anomalies, in which an elongated transverse process of the concluding lumbar vertebra fuses with varying degree to the "get-go" sacral segment.ane LSTV, equally a morphological variation, spans a spectrum from partial/complete L5 sacralization to partial/complete S1 lumbarization.2, iii When the L5 vertebra fuses completely to the sacrum, 4 lumbar vertebrae exist, whereas when S1 separates entirely from the sacrum, 6 lumbar vertebrae exist and the sagittal contour of the spine becomes more lordotic.four Many intermediate incomplete transitions accept also been recognized and classified every bit LSTV.5
Castellvi et al. classified LSTV into four types (Figure one). Blazon I includes unilateral (Ia) or bilateral (Ib) dysplastic transverse processes, measuring at least 19 mm in width (craniocaudad dimension). Type Two exhibits incomplete unilateral (IIa) or bilateral (IIb) lumbarization/sacralization with an enlarged transverse process that has a diarthrodial articulation between itself and the sacrum. Blazon Iii LSTV describes unilateral (IIIa) or bilateral (IIIb) lumbarization/sacralization with complete osseous fusion of the transverse process(es) to the sacrum. Type IV involves a unilateral type II transition with a type Iii on the contralateral side.3, 6
Estimates of the prevalence of LSTV in the full general population vary widely throughout the literature due to differences in definition and diagnostic modalities, ranging from 4.0% -35.ix% with a mean of 12.three%.3, 5, 7, viii In a study of 211 participants, Apazidis et al. adamant Type IA most common with a prevalence of fourteen.7%;vii nevertheless, Type I is generally considered to have no clinical significance and does not crave farther attention in clinical exercise.6 In an asymptomatic population, Nardo et al. determined that Type I and Type II were each responsible for more than 40% of full occurrences of LSTV, while Type III and Type IV accounted for eleven.5% and 5.25% of occurrences, respectively.ix In unilaterally occurring malformations, the incidence is significantly higher on the left side, a finding which remains unexplained.10
The prevalence of LSTV is higher in men compared to women (28.1% vs. xi.1%).9 Sacralization is more than common in males, meanwhile accessory L5-S1 articulations and lumbarization of S1 are more common in women.11 Cases of families with increased incidence of LSTV propose a genetic component.12 HOX10/HOX11 genes influence centric pattern of lumbar and sacral vertebrae. Mutations in these genes may play a role in the formation of LSTV.v
Anatomical Variations
The presence of an LSTV disrupts normal spine biomechanics and anatomy. The sacrum, lying at the base of operations of the vertebral column, optimizes the dissipation of the weight of the upper torso toward the sacroiliac (SI) articulation past working equally a fused mass of boney elements.11 The sacrum'south power to misemploy load depends on its size and its surface area with the SI joint. Although HOX genes regulate segmentation of the vertebral column into individual vertebral segments, germination of transitional states at the lumbosacral junction may be greatly influenced by the functional requirements of load manual at the SI junction. According to cadaver studies, sacra incorporating L5 possess significantly smaller heights than the normal sacra if the fused L5 vertebra is excluded from the measurement. This procedure of "add-on" or "diminution" of segments to or from the sacrum depends on the load-begetting capacity of the normal (S1-S5) sacrum at a very rudimentary stage of its germination. Therefore, a small sacrum with inadequate SI joint expanse may incorporate L5 to enhance load-bearing capacity, while a sacrum with over competent load begetting capacity may release S1.13
Boney abnormalities associated with LSTV touch surgery in the lumbosacral region. In the case of sacralization, all dimensions, including pedicle superlative, sagittal and transverse dimensions, and sagittal angulation are reduced, and downwards slope is increased. xiv The height of the pars interarticularis (PI) and the widths of laminae are significantly smaller in the last lumbar segment of sacralized specimens. Small PI may predispose spondylolysis and spondylolisthesis at lumbo-sacral junctions associated with transitional variations, and warrant special attending to avoid iatrogenic injuries.15 Lumbarization of S1 results in a shorter altitude between facet and sacral promontory, more than obtuse pedicles in the sagittal plane and less steep in front. Therefore, pedicle screws should be directed more obtusely in the sagittal aeroplane and at a reduced downward inclination.14 LSTV possess a reduced number of trabeculae of cancellous bone. Consequently, spiral placements and subsequent pullouts should be reviewed.16
LSTV showroom contradistinct articular facets at the L5-S1 junction such that the facets are smaller and more coronally oriented. Lumbarization results in the smallest facet linear dimension, smallest surface area, and maximal coronal orientation. Sacralization demonstrates insignificant alteration in facet morphology. Facet asymmetry is predominantly associated with accessory L5-S1 articulations, but is seen in all LSTV subtypes. These alterations are possibly related to low back pain situations.17
The clan betwixt LSTV with morphological alterations of neural curvation elements and auricular surfaces is well established. Considering the biomechanical importance of these morphological alterations in maintaining stability of the lumbar spine, Mahato suggests re-defining and modifying the current nomenclature of LSTV. Including facet and auricular surface status would allow clinicians to clearly delineate the entire range of information required to visualize and clinically interpret whatever subtype of LSTV illness (Table 1).two
Table 1
Redefining lumbosacral transitional vertebrae (LSTV) classification through integrating the full spectrum of morphological alterations in a biomechanical continuum.2
The disc height below a lumbosacral segment is significantly decreased in LSTV types Ii, Three, and IV.xviii, 19 The presence of a bilateral boney fusion decreases disc top more than severely compared to segments with potential for motion (unilateral fusion). The mutual finding of a narrowed L5-S1 intervertebral disc associated with an LSTV should non exist considered disk degeneration or displacement.19 In improver, the sagittal alignment is well-nigh commonly neutral, different the typical lordotic L5-S1 disc.
In an anatomical study of 70 cadavers, Aihara et al. found that the iliolumbar ligaments at the level immediately above transitional vertebrae are thinner and weaker than those in cadavers without LSTV. The weak iliolumbar ligaments result in vertebral segment instability and could later on pb to early disc degeneration. The formation of an joint or boney union between vertebra and sacrum through the transverse procedure may stand for an adaptive machinery to compensate for a weak iliolumbar ligament and to preserve stability.20
LSTV touch on the terminal level of the conus medullaris (TLCM). Compared to controls, the TLCM is significantly higher in the presence of a sacralized L5 and significantly lower in the presence of a lumbardized S1. This finding may help clinicians place the neurological discrepancies observed among neurologic injuries at the thoracolumbar junction. 21
In 1980, McCulloch and Waddell proposed that the functional L5 nerve root e'er originates from the "last mobile" segment of the spine. The concluding mobile segment of the spine is defined as the lowest level with a fully formed disc space, bilateral facet joints and two free transverse processes which do not articulate with the ala of the sacrum or the pelvis. Therefore, in the case of a sacralized L5, the functional L5 nerve root corresponds to the anatomical L4 nerve root. In patients with a lumbardized S1, the last fully mobile level is usually L6-S2, and the functional L5 nerve root corresponds with the L6 nerve root.22 Chang et al. agreed, terminal that neurologic symptoms caused by the L6 nerve root compression resemble those of the L5 rather than the S1 nerve root compression in the normal configuration. 23 In 2008, Kim et al. suggested in the case of lumbardized S1 (L6), the distribution of motor and sensory symptoms caused past the lumbardized S1 (L6) nerve root stimulation is similar to that of the S1 nervus root stimulation in the normal configuration.24 Furthermore, Hinterdorfer et al. implemented intraoperative electrophysiological monitoring by ways of evoked EMG to compare segmental innervation in patients with 5LVB and 6LVB. This written report provides strong evidence that the function of the lumbosacral nervus root is not significantly altered in patients with 6LVB, significant that the L6 nerve root is equivalent to the S1 nerve root in patients with 5LVB. In add-on, the root emerging from L6/South not simply primarily resembles the S1 root merely also shows characteristics of the S2 nerve, with a trend to innervate the biceps femoris muscle.25 Seyfert, with careful use of cremasteric reflex, concluded that lumbarization shows a dermatome gap between the lumbar dermatomes C1-C3 and the sacral dermatomes S2 and S3, which lay significantly more than ventral than in patients with a normal spinal configuration.26 The alteration in nerve root innervation caused by a transitional vertebra may make it hard to find the pain generator. Therefore, in patients receiving epidurals or selective nervus root blocks, one should exist aware of a transitional segment before initiating the injection. 24
Lumbardized sacrums represent a relative contraindication for lateral transpsoas interbody fusion at L5-six due to migration of neural anatomy within the psoas musculus. Smith et al. reported that eight out of 10 patients with half dozen lumbar vertebrae were converted to an alternative arroyo later on a corridor through the psoas muscle was not found. Axial MRI reveals a teardrop-shaped psoas discrete from the lateral border of the disc infinite in patients with transitional anatomy unapproachable at L5-6, resembling L5-S1 in normal anatomy. Preoperative axial MRI and intraoperative advanced neuromonitoring can help avert injury.27
Surgeons must consider the likelihood of vascular variation in the presence of an LSTV. According to Weiner et al., 11 out of 12 patients undergoing anterior lumbar interbody fusion at the functional junction above a fixed transitional level required significant alteration of the approach secondary to vascular variation. The more caudal location of the junction betwixt the common iliac veins and the inferior vena cava prohibits safe access to the functional L5-S1 disc below this junction. Accordingly, an approach lateral to the junction with mobilization of the left common iliac vein and inferior vena cava to the right of the midline is virtually always required, similar to the arroyo to the L4-L5 disc.28
Clinical Significance
Low dorsum pain in the presence of an LSTV was originally noted by Mario Bertolotti in 1917 and termed "Bertolotti'south Syndrome". According to Quinlan et al., the prevalence of Bertolotti's syndrome is 4.six% in the general population and 11.four% in patients under the age of thirty.29 Among 8280 patients seeking care for low back hurting, Paik et al. institute x.half dozen% had LSTV types II, III, or IV, with sacralization bookkeeping for 5.iii% and lumbarization bookkeeping for 5.3%.5 Throughout the literature, the prevalence of LSTV in patients seeking intendance for depression back hurting ranges from 4.six%-35.vi%.seven, 29 Due to its broad prevalence, Quinlan et al. encourages physicians to consider Bertolotti'due south syndrome in the differential diagnosis for low back pain, especially in younger patients.29
The potential association between LSTV and low dorsum pain has been debated since it was first described by Bertolotti almost a century ago.5 Amid 4636 patients from the Osteoarthritis Initiative (OAI) cohort, Nardo et al. found that 53.9% of the patients without an LSTV reported low back pain. 46% of patients with a Type I and forty% of patients with a Type 3 LSTV reported low back pain, suggesting these anomalies might be a protective factor. 73% of patients with Type Ii and 66% of patients with Type IV LSTV reported low back pain. Blazon II and Type IV LSTV positively correlate with increased prevalence and greater severity of low back and buttock pain and with lower physical activeness levels.9, 30 Tang et al.'s contempo written report of 928 individuals with LSTV supported the association between Type 2 LSTV with low dorsum and gluteal hurting, with corresponding odds ratios of 2.56 and 5.38. The odds ratios for low back and gluteal pain given the presence of a Type IV LSTV are 4.28 and 6.82, respectively.8
Conversely, other authors believe that lumbosacral transitional segments are quite common in the general population and may not be seen with higher prevalence in patients reporting low back pain.7 In 1977, Tini et al. institute an insignificant difference betwixt incidence of LSTV in patients with depression dorsum pain (6.7%, n=4000) and in the full general population (five%, n=1873).12 Several other studies found similar outcomes, concluding no difference in pain, disability level or neurological signs between individuals with and without an LSTV.7, 18, 31–33
A third opinion suggests that depression back pain complaints might be worse, simply not more frequent in the presence of an LSTV. Worse hurting may result from the concentration of external stress on adjacent vertebral levels.34, 35 Among 881 immature male patients, Taskaynatan et al. reported that the presence of an LSTV increased the severity of the patient's clinical pic and severity of pain.34 According to Yavuz et al., subjects with low back pain and no malformation reported an average pain level on the Visual Analog Scale for Pain (VAS) of 2.2 versus four.8 in patients with depression back pain and a transitional vertebra.35
Structural Pathologies
Bertolotti stated equally early as 1917 that an LSTV may produce low back pain due to arthritic changes occurring at the site of pseudoarthrosis.36 Hurting in the presence of an LSTV may likewise arise from disc herniation or degeneration, facet joint arthrosis, or spinal canal or foraminal stenosis.5 In 1989, Elster et al.'southward radiographic study of 2000 patients suggested that the overall incidence of structural pathology, including significant disc protrusion, nervus root canal stenosis, spondylolysis, and sclerosis at "false joints" is not appreciably higher in LSTV patients than in patients without such vertebrae.37
Avimadje et al. found 52.seven% of patients with a lumbar disc herniation also had an LSTV, while just eighteen.iii% of the control group had an LSTV.38 Among patients with unilateral LSTV, 75.9% of the lumbar disc herniations occurred on the aforementioned side as the transitional vertebrae.39 Patients with a transitional vertebra experience disc herniation more oftentimes (17% vs. xi%) and at a younger age (35 years former vs. 59 years old) compared to patients without a transitional vertebra. 32 Since historic period-related degenerative changes are common in the disc above a normal L5, the effect of transitional vertebrae may be obscured in middle age. The possible increased prevalence of disc protrusion or extrusion in a higher place the transitional vertebra could lead to radiating hurting every bit a result of nervus root compression and chemical irritation.18
The probability of finding LSTV in patients with clinically significant spinal symptoms is 1.75 times higher than in patients with non-spinal complaints. This probability increases to two.3 times amid patients with symptoms severe enough to require an MRI and increases to iii.6 times among patients with last mobile disc herniation requiring discectomies. Therefore, it is possible to conclude that LSTV are more probable to exist present in patients with clinically meaning spinal symptoms and even more so in those operated on for disc herniation of the terminal mobile disc.40
Although the clan between LSTV and pain continues to be debated, universal agreement throughout the literature describes an altered pattern of degenerative changes in patients with LSTV. Hypermobility and abnormal torque moments at the level immediately to a higher place the transitional vertebra and restricted move between the L5 and S1 vertebra result in degenerative changes at the level above the anomalous joint.18, 20 Disc protrusion and/or extrusion occurs more often at the level supradjacent to the LSTV than at the aforementioned level in patients without an LSTV (45.3% vs. 30.iii%). This is also true for disc degeneration (52.8% vs. 28%), facet degeneration (60.iv% vs. 42.six%) and nerve root canal stenosis (52.eight% vs. 27.9%).41 Otani et al. reported 83% of patients with a disc herniation in the presence of an LSTV experienced symptoms arising from the terminal caudal mobile segment. Patients with disc herniation and no transitional vertebrae nearly frequently (59%) had symptoms arising from the 2nd final mobile segment. 32
Disc bulge or herniation is exceedingly rare at the interspace below a transitional vertebra.20, 23, 32, 37, 39, 42 Increasing the mechanical connection of a lumbosacral transitional vertebra protects the disc at the transitional level. The greater the osseous bridging at the transitional level, the more the transitional disc seems to exist preserved from degeneration.43 The protective effect of transitional vertebrae acts stronger on the annulus fibrosus than on either the nuclear complex or endplates. Overall, the effect of transitional vertebrae on the next discs may mimic the situation subsequently a fusion operation when movement at one or more disc spaces is restricted in relation to other disc levels.18
The incidence of spinal stenosis and spondylolysis is not significantly college in patients with an LSTV.37, 44 Nevertheless, the presence of an LSTV makes the magnitude of anterior slippage more severe. The greatest average slippage of L4 (nineteen.three%) occurs in sacralized patients. In lumbardized patients, the boilerplate slip of L4 is xiv.5%, while in control groups, the average slip of L4 is11.4%.45
Unilateral LSTV upshot in asymmetrical biomechanical alterations. The side bearing the additional L5/S1 human relationship supports a larger proportion of load, resulting in lateral tipping of the iliac crest and convexity of a scoliotic curve towards the side of the articulation. The sacroiliac joint on the side of the LSTV will increase the auricular area, probably resulting in increased loading of that articulation, greater wear and irritation of the joint, greater fixation on exam, and increased one sided musculus activity.46 Asymmetry tin can cause early on degenerative changes within the normal contralateral facet joint, giving ascension to facet pain.47 Furthermore, asymmetrical motion may also influence disc degeneration.48
In Type II LSTV, the pseudoarticulation between the transverse procedure and the sacrum creates a "false articulation", in which degenerative changes have occasionally been noted in clinical studies.46 The presence of sclerotic changes and osteophytes near the faux articulation imply slight movement in these vertebrae. Initial studies suggested that the side with degenerative changes in the joint between the transverse process of the transitional vertebra and the pelvis practice not correlate with the side of pain.37 More recently, however, Connolly et al. demonstrated that 80% of young patients with depression back pain and an LSTV had loftier uptake on os scintigraphy at the transverse-sacral joint. The transverse-sacral articulation was the merely abnormality in 63% of these depression back pain patients, suggesting that localized stress at the articulation contributes to low back pain.49
S1 lumbarization has been implicated in pinch neuropathy of the S1 nerve root.13 The presence of an LSTV can consequence in pinching of a lumbar spinal nerve betwixt the transverse procedure of the 5th lumbar vertebra and the sacral ala, a status known as "Far-Out Syndrome."50–52 Osteoporosis resulting from "micromotion" at dysplastic facet joints at the level beneath the transitional vertebra can result in extraforaminal entrapment of the spinal nerve leading to radiculopathy.50 Neural compression by new bone formation below an LSTV occurs with a reported prevalence of xiii% and tin be symptomatic in up to 70% of these patients.53
Imaging Lumbosacral Transitional Vertebrae
Most incorrect level surgical procedures occur in patients with numeric variant spines and/or LSTV.12 Spine physicians and radiologists must consider the possibility of numeric and morphological variations in lumbosacral images in order to avoid intervention or surgery at the incorrect level.42 To make up one's mind the location of a specific vertebral body on a sagittal radiograph, the last vertebra with a rectangular shape is mostly considered to be L5, so the vertebral bodies are numbered from the bottom to the meridian. Nevertheless, in the presence of an LSTV the rectangular shaped concluding vertebra can exist L4 or L6.five
The xxx° angled AP radiograph (Ferguson radiograph) serves every bit the reference standard method to notice LSTV (Effigy two). Sagittal images highlight transitional lumbosacral anatomy, such as "squaring" of the transitional vertebral body and reduced peak of the transitional disc (Figure 3). Axial images draw pseudoarthrosis or fusion of the terminal lumbar vertebra with the sacrum.1
- Download figure
- Open in new tab
- Download powerpoint
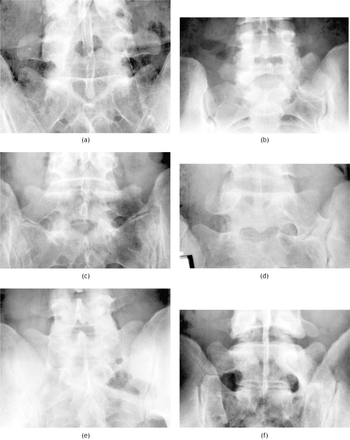
Fig. two
Appearances of LSTV based on Castellvi et al. (a) Blazon 1b with bilaterally enlarged L5 transverse procedure simply no articulation with the sacrum. (b) Type 2a with unilateral pseudarthrosis. (c) Type 2b with bilateral pseudarthroses. (d) Blazon 3a with unilateral fusion of the enlarged transverse procedure to the sacral ala. (eastward) Type 3b with bilateral fusion. (f) Type 4 advent with fusion on the left side and a pseudarthrosis on the right.i
Standard AP radiographs demonstrate 76%-84% accuracy for LSTV detection and 53%-58% accurateness to classify LSTV. Diagnostic errors in identification of vertebral levels on sagittal lumbar MRI are also mutual. 43 According to Tokgoz et al., 1.iii% of patients with normal sectionalization were misdiagnosed on MRI as having an LSTV, 35.ane% of the patients with an LSTV were misdiagnosed equally having normal segmentation, and lx% of the patients with a correctly diagnosed LSTV had an incorrect number of vertebral levels.54
O'Driscoll et al. classified four types of lumbosacral junctions based on sagittal T1/T2 lumbar spine MRIs. In Type i no disc material is present. Blazon 2 denotes a small residuum disc not extending for the whole AP bore of the sacrum. Type three represents a well-formed disc extending for the whole AP bore of the sacrum, while Type 4 is identical to Type 3 only with an aberrant upper sacral outline coordinating to the "squaring" appearance on sagittal radiographs. Blazon 4 correlates with a fused LSTV (Castellvi Blazon III or Type IV).55 Furthermore, Desmond et al. utilized sagittal T2-weighted spinecho MRI in patients with LSTV to classify the transitional disc as Type i or Blazon two. A Type 1 transitional disc is smaller than the disc at the next mobile segment, maintains T2-weighted betoken intensity, lacks an intra-nuclear scissure, shows no evidence of fusion between anterior vertebral body endplates and associates with the pseudoarthrosis of the transverse vertebra of the LSTV to the sacrum. A Blazon ii transitional disc is smaller than Type one, maintains its signal intensity, lacks an intra-nuclear scissure, shows bear witness of anterior endplate fusion and concave endplates to the disc and is associated with the complete fusion of the LSTV to the sacrum.56
LSTV patients often demonstrate exaggerated lumbar lordotic curvature and a lack of sharp angulations at the lumbosacral junction on mid-sagittal MRI. An angle formed by a line parallel to the superior surface of the sacrum and a line perpendicular to the axis of the scan table on mid-sagittal T2-weighted MRI >39.8° predicts the presence of an LSTV with 80% sensitivity and eighty% specificity. In addition, an bending formed by a line parallel to the superior endplate of the L3 vertebra and a line parallel to the superior surface of the sacrum >35.9° predicts the presence of an LSTV with lxxx% sensitivity and 54% specificity. 48 It should be noted that the magnitude of the angle formed betwixt the lumbosacral junction vertebral endplates (lumbosacral intervertebral disc angle) is non a useful diagnostic tool.57
Farshad et al. advocate measuring the differences per segment of the vertical mid-vertebral angle (Unequal-VMVA) and the vertical anterior vertebral bending (Diff-VAVA) of the three about caudal segments of the lumbar spine to simply and reliably identify LSTV. A Unequal-VMVA of ≤ +x° identified type III and Iv LSTV with a sensitivity of 100% and a specificity of 89% on MRI and with a sensitivity of 94% and a specificity of 74% on lateral radiograph. In terms of Unequal-VAVA, a sensitivity of 100% and a specificity of 76% were achieved with a cut-off value of 28°.58
Paik et al. suggest routinely calculation sagittal T2W images to the lumbar MRI protocol and thoracolumbar sagittal T2W images to the cervical MRI protocol. In addition to screening of coexisting lesions, wholespine sagittal T2W images play an essential part in authentic vertebral numbering. Numbering caudally from C2 on whole-spine MR images and utilizing morphological classification by Castellvi enables proper identification of both numeric and morphological vertebral variations (Figure 4).v Manifestly radiographs of the thoracolumbar junction enable hypoplastic truthful ribs to exist differentiated from big transverse processes and therefore enable correct identification of the L1 vertebral body.22, 57
- Download figure
- Open in new tab
- Download powerpoint
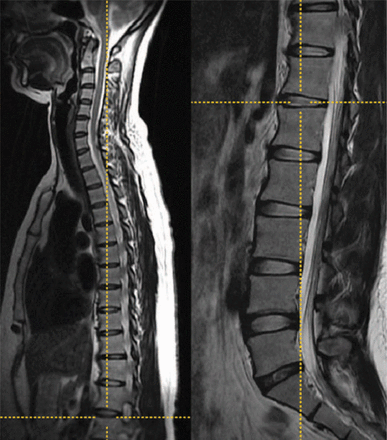
Fig. 4
A case of L6 vertebra with type IIa transition. Left, T2-weighted sagittal cervicothoracic and (right) lumbar images in the cross-referencing fashion of the motion picture archiving and communication system. This simultaneously demonstrates the marker at the T12–L1 disc infinite. Counting the vertebral levels caudally from C2 reveals this patient to have 25 presacral vertebrae or 6 lumbar vertebrae.five
Milicic et al. propose that the suspicion of an LSTV in a child requires sagittal images of the sacrum and coccygeal os on T2 weighted sequence in addition to MR imaging scans of the lumbosacral spine. The clinician should count upward from S5 and precisely make up one's mind S1. Determination of S1 enables detection of the L5 and, in plow, all other vertebrae.59
Paraspinal structures in positions outside their frequent location may signify the presence of a transitional vertebra. On sagittal images, the aortic bifurcation, IVC confluence, right renal avenue, celiac torso, and superior mesenteric avenue root are located one-3 levels more than caudal than normal in the case of lumbarization, and 1-3 levels more cephalic than normal in the case of sacralization.60 Nonspinal anatomic landmarks are problematic, however, because of their variable location and potential changes with age.57
Although Hughes et al. concluded that the iliolumbar ligament always arises from L5,61 a more accurate conclusion of their research would exist that the iliolumbar ligament arises from the concluding lumbar vertebra, which could be L4, L5, or L6, depending on the sectionalisation of the spine.62 Therefore, the iliolumbar ligament does not permit for absolute numbering of the vertebral column and the iliolumbar ligament is non a consistent tool to number the spine, as it does non ever signal the L5 level.57
An anomalous number of presacral vertebrae is 7x more likely in the presence of an LSTV. In addition, the presence of an LSTV is associated with a higher incidence of a concomitant thoracolumbar Tv (TLTV) and vice versa. Identification of an LSTV should prompt additional imaging to verify numbering, peculiarly if an intervention is contemplated. Clinicians should remember that no landmark is consistentlyreliable, so an explicit statement regarding how the lumbosacral junction was determined must exist made in the imaging report.57
Diagnosis And Treatment Of Bertolotti'S Syndrome
Low back pain is a prevalent trouble with multiple causes. Approximately 80% of adults seek a physician's aid for low back pain at some bespeak in their lives. Given the broad prevalence of LSTV, it is important that low back pain in the presence of an LSTV is not automatically attributed to the radiographic finding of an enlarged transverse process.63 A diagnosis of Bertolotti's syndrome should exist charily considered with appropriate patient history, imaging studies, and diagnostic injections.64 Equally with other causes of low back hurting, the initial treatment of symptomatic LSTV is clinical, including a combination of NSAIDS and rehabilitative concrete therapy.65 There is a lack of consensus, however, regarding the handling of this condition, and the number of studies and case reports in the literature reporting on the diagnosis and outcomes of patients with symptomatic LSTV is sparse.64, 66
The literature includes 4 reports of either chiropractic management or physical therapy to care for symptomatic LSTV. Muir et al. reported 2 patients with Castellvi Type IIa LSTV presenting with limited ipsilateral flexion coincided with ipsilateral muscular symptomatology similar to piriformis syndrome. ane patient experienced 70% improvement in symptoms after 2 weeks of spinal manipulation, soft tissue therapies, exercise and stretching. The other patient reported improvement in pain and perceived mobility after iv weeks of similar treatment.66 2 additional case reports described patients with low back hurting and an LSTV that resolved following spinal manipulation, stretching and exercise.67, 68 The authors proposed that the decreased mobility at the L5/S1 junction brought on past an LSTV results in biomechanical changes and contradistinct weight distribution at this level. These changes increase stress on the muscles in the region of the sacroiliac and lumbosacral junction on the afflicted side. Therefore, the authors indicated a office for conservative intendance in patients with LSTV, not to relieve force per unit area on an impinged nerve, only instead to address muscular alterations in the lumbopelvic musculature.66
Because of its simplicity, low expense, and wide availability, functional flexion-extension radiography is the near thoroughly studied and the most widely used method in the imaging diagnosis of lumbar intervertebral instability. Flexion-extension lateral views allow measurement of the sagittal translation of a vertebra with respect to the underlying one and the corporeality of vertebral rotation in the sagittal airplane.69 According to Little et al., strengthening and stabilizing exercises probably have moderate benefit on patients with low back hurting associated with abnormal motility patterns identified on dynamic x-ray studies.70 Lessons in the Alexander technique offer an individualized approach to develop skills that help patients recognize, sympathise, and avoid poor habits affecting postural tone and neuromuscular coordination. Little et al. randomized 579 patients with recurrent low dorsum pain to normal care, to 6 Alexander technique lessons, or to 24 Alexander lessons. 24 lessons in the Alexander technique taught by registered teachers provided long-term benefits for patients with chronic or recurrent low back pain. The authors reported changes in postural tone and changes in load and position. These findings supported the hypothesis that the Alexander technique could potentially reduce back pain by limiting muscle spasm, strengthening postural muscles, improving coordination and flexibility, and decompressing the spine.70 Several studies take likewise examined the effects of Pilates method in people with chronic depression back hurting. The literature defines Pilates method equally a mind-body exercise that focuses on core stability, muscle control, animate, strength, flexibility, and posture. Pilates method involves conscious employ of torso muscles to stabilize the pelvic-lumbar region. The current consensus suggests that Pilates methodbased exercises are more effective than no treatment or minimal physical do interventions in the management of chronic low back pain.71
L4/5 articulation radiofrequency sensory ablation has been reported to provide 100% relief of buttock pain for 16 months in ane patient with an LSTV.72 Additionally, Endo et al. reported firsthand disappearance of low back pain in a patient with an LSTV following electric denervation of the infinite betwixt the transverse process of the 5th lumbar vertebra and the sacral ala. The authors advocated electric denervation every bit a minimally invasive and potentially effective method for pain eradication.73
Injections of steroids or local anesthetics into the transverse process pseudoarticulation site can exist both diagnostic and provide immediate, albeit temporary, pain relief.64 Almeida et al. advocated performing these blocks with a minimal amount of anesthetic delivered precisely to the betoken of involvement.65 Mitra et al. reported an improved Oswestry score from 33 to 26 in a 64-yr-one-time female with a Type IIb LSTV 1 month following a local anesthetic and corticosteroid injection administered to the transverse process-ilium joint.74 In a retrospective study of 12 patients with unilateral lumbo-sacral anomalous articulation with aforementioned side low back or buttock hurting, 9 patients reported a l% decrease in pain after 1 month. vii out of eight patients who were re-evaluated 24 months later on improved or were symptom free.38 Marks et al. reported that 7 out of 10 patients with chronic depression dorsum pain and an anomalous lumbosacral articulation obtained worthwhile relief after steroid injection of the anomalous lumbosacral articulation and ane patient remained pain free at 24 months.75
A diagnostic injection at the pseudoarticulation site not only provides pain relief but as well helps determine if the LSTV is a significant source of the patient's depression back pain and radicular symptoms. Li et al. relied on patient response to injection as an exclusionary examination for surgery. Specifically, if the injection did non provide relief, the patient was non considered a surgical candidate. Discography may be useful if the disc above the transitional vertebra is thought to be the source of the pain.63
Bone scintigraphy complements the evaluation of patients with low back pain idea to arise from LSTV articulations. LSTV articulations increase uptake on bone scintigraphy secondary to degeneration and metabolic activity of the anomalous articulation (Figure 5). Pekindil et al. evaluated 28 patients in whom a lumbosacral transitional vertebral joint had been identified radiographically. On planar imaging, normal-to-minimally and normal-to-moderately non-focal increased uptake was observed in patients without degenerative changes and with degenerative changes, respectively. The authors stated that when increased uptake is seen on the upper 1/2 to ane/iii role of the sacroiliac joint on planar images, this should not be mistaken for sacroiliac articulation affliction and degenerative LSTV articulations should especially be considered in the differential diagnosis. On SPECT imaging, the patients who had no degenerative changes at the anomalous articulation had non-focal mild uptake. However, in symptomatic patients with degenerative changes in which no crusade was found for depression back pain past clinical, laboratory, CT and bone SPECT examinations, there was focal markedly increased uptake on SPECT imaging. The authors advocated that focal, markedly increased uptake may testify the metabolically active degenerative changes of LSTV joint and may aid to reveal pain arising from LSTV articulations.76
- Download effigy
- Open in new tab
- Download powerpoint
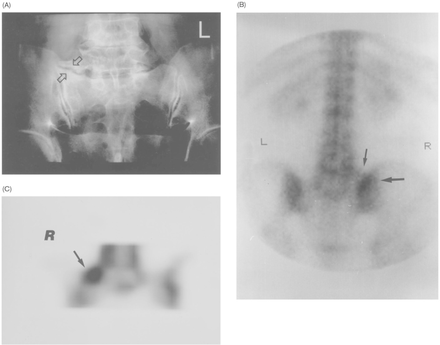
Fig. 5
Female patient historic period 62 with low back pain and with degenerative type IIA LSTV articulation (arrows) on the correct side on plain motion picture. (B) Non-focal, moderately increased uptake (large arrow) on the upper sacroiliac joint expanse at the planar scan. Note also the non-focal, minimal, tracer activity (modest pointer) corresponding to the right enlarged transverse process. (C) Coronal SPECT image demonstrates focal, markedly increased activity (arrow) located in the degenerative dissonant articulation expanse. This patient was diagnosed equally having active degenerative disease.63
Almeida et al. proposed a diagnostic-therapeutic algorithm based on the clinical and surgical experience they caused treating 5 patients with low back pain in the presence of an LSTV (Effigy 6). These five patients did not improve with clinical treatment, including non-steroidal anti-inflammatory drugs (NSAIDS), physiotherapy and physical exercises. The patients were submitted to an coldhearted block at the contact of the mega-apophysis with the sacrum, which provided temporary pain relief in all v patients. Thereafter, they underwent radiofrequency neurolysis, whereby 3 patients experienced only a fractional command of the pain and 2 experienced pregnant improvement. The latter ii patients underwent mega-apophysis surgical resection and achieved complete resolution of symptoms during the 1 twelvemonth follow upward. The authors recommended considering mega-apophysis surgical resection for the sub-group of patients with low back pain and LSTV who neglect conservative treatment, merely feel temporary relief with coldhearted block. Other associated causes of low back pain should be considered if anesthetic block of the anomalous articulation does not provide pain relief.65
Jonsson et al. described 11 patients with low back pain ipsilateral to an LSTV. None of the patients had signs or symptoms of lumbar nerve root compression. 9 out of the 10 patients who had an injection of local anesthetic into the dissonant articulation experienced pain reduction or alleviation. These 9 patients afterwards underwent resection of the abnormal joint. At 6 to 42 months postoperatively, 7 patients reported full alleviation of pain, and 2 experienced significant comeback.77
Santavirta et al. surgically treated 16 patients with radiographically diagnosed LSTV and chronic, persistent low back pain with either posterolateral fusion or resection of the transitional articulation. ten of the 16 operatively treated patients showed improvement of their low back pain. The results were similar in the group treated with fusion and in the grouping treated with resection. 11 patients had persisting episodes of sciatica (versus 13 preoperatively). At follow-up the first disc above the fused segment was found to be degenerative in vii out of viii cases, and in the group treated with resection the outset disc to a higher place the transitional vertebra was degenerated in 5 out of 8 cases. 3 patients from each group were treated with 2nd operations. Compared to 16 conservatively treated controls, the operatively treated patients had slightly better Oswestry pain scores, even so the total Oswestry disability scale scores did not differ. Given that the results of surgical treatment were simply slightly improve than conservative handling, the authors suggested operative treatment in only very select patients who should be carefully examined for disc pathology. The authors recommended resection if the patient's pain can be definitively attributed to the transitional joint, conservative treatment fails, and no disc pathology tin can be detected. Posterolateral fusion may exist considered if the transitional disc is degenerated, and the disc above the transitional vertebra is intact.78
Ugokwe et al. achieved 97% pain resolution in one patient with a minimally invasive approach to resect an enlarged transverse process and the accompanying anomalous pseudoarticulation at the L5 level. The aforementioned authors published the results of vii patients who underwent minimally invasive paramedian tubular-based resection of symptomatic LSTV. The hateful age at the time of surgery was 43.iii years and the mean age at diagnosis of Bertolotti's syndrome was 40.2 years. The median duration of low-back hurting and/or radicular symptoms was eight years prior to surgery. three of 7 patients reported complete resolution of low back pain, two of 7 patients had reduced low-dorsum hurting, and ii patients experienced initial relief but render of low-back hurting at 1 and four years postoperatively. iii of the half dozen patients with radicular pain had consummate relief of this symptom.64
Only 8 cases of impingement of a nervus root by a bony spur at the articulation betwixt the transverse procedure of a transitional vertebra and the sacrum have been reported in the literature. 6 of these patients underwent surgical intervention. In a patient described by Abe et al, MRI revealed mild degenerative changes with minimal posterior disc bulging and impingement of the left L5 nervus root by bony spur formation at the anterior go out zone of the nerve root foramen below a transitional vertebra. Selective nervus root sheath infiltration of the left L5 nerve root was performed. The patient's pain was reproduced over the same area of the left leg during insertion of the needle. Immediately later the injection of a 2-mL solution of two% lidocaine hydrochloride with contrast, these symptoms completely disappeared. Selective radiculography demonstrated foraminal impingement of the nerve root between the lateral bony spur and the medial intervertebral disc. Given that 3 lesions demonstrated past MRI could have been the symptomatic lesion, selective radiculography proved useful in differentiating the symptomatic lesion of the nerve root. The authors and so performed an inductive decompression (left-sided, muscle splitting, extra peritoneal arroyo/Fraser's Incision), which resulted in consummate resolution of back pain and numbness by the follow-upwards exam i year after surgery.51 Kikuchi et al reported two additional cases of inductive decompression for far-out syndrome beneath a transitional vertebra. Inductive decompression was performed for both cases using a Fraser incision and resulted in successful resolution of symptoms. The authors advocated anterior decompression for cases of far-out syndrome refractory to selective nerve root block, explaining that this approach allows for a more complete decompression in the context of entrapment more than anterior of the exit zone of the foramen compared to other pathologies. The authors stated that it would have been difficult to obtain a wide, well-illuminated, and dry surgical field from the posterior approach.51, 79
Ichihara et al. however, reported no difficulty with decompression using a posterior arroyo for ane patient who obtained skilful relief of radicular pain. The authors described posterior decompression as an piece of cake, prophylactic, and useful treatment for radicular pain acquired by an L5 nervus far-out syndrome when conservative treatments fail to obtain proficient relief.52Weber and Ernestus reported a patient with radicular pain and a unilateral bibelot of the correct transverse procedure of L5 resulting in foraminal stenosis of the L5 spinal nerve and, specially, entrapment exterior the foramen between the big transverse process of the sacral ala. Following foraminal and extraforaminal decompression of the nerve via an extraforaminal arroyo, the patient reported no radicular or lumbar pain at 12 months follow up.l Miyoshi et al. employed selective radiculography and nerve root block followed by computed tomography to highlight foraminal entrapment of the L5 nerve root via osteophytes below a transitional vertebra. The patient underwent posterior decompression past resection of the osteophytes using an operating microscope and the patient experienced skilful relief of radicular pain. The authors emphasized that selective radiculography is the most reliable modality to diagnose far-out entrapment of the L5 nerve root and that CT in combination with radiculography clearly demonstrates not only the degree of L5 nervus root impingement, but besides the etiology of the L5 nerve root compression.80
Shibayama et al. described a patient with an enlarged right-sided transverse process at L6, moderate compression of the dural sac on the right side at L5-6, and mild compression of the right L6 spinal nervus. Although microendoscopic decompression of the spinal canal provided little relief, extraforaminal decompression of right L6 relieved both low dorsum hurting and sciatica. The authors suggested that intractable sciatica secondary to an enlarged transverse process could arise from impingement of the nervus root extraforaminaly rather than between the transverse procedure and the sacrum.81 Information technology is ofttimes difficult to differentiate symptomatic and asymptomatic extraforaminal stenosis secondary to osteophyte formation on conventional MRI alone. With the use of 3D MR lumbosacral radiculography, Byun et al. associated indentation or swelling at the L5 nerve root with symptomatic extraforaminal stenosis. These radiographic findings were distinctively absent in cases of asymptomatic extraforaminal stenosis.82
Resection of a right-sided unilateral anomalous lumbosacral articulation provided 90% relief of left depression back pain and complete relief of left leg symptoms in 1 patient with a contralateral symptomatic L6-S1 facet joint. The authors suggested that the patient's pain was not associated with the anomalous joint itself, only was probably due to additional stress placed on the normal contralateral joint. In this example, hurting relief resulted from reduced stress on the symptomatic facet.47
Conclusions
Although Bertolotti's syndrome was get-go described nearly a century ago, fence continues regarding the prevalence, clinical significance, radiographic identification and treatment of symptomatic LSTV. While early studies depicted LSTV equally a rare anatomical anomaly, studies incorporating revised definitions and improved imaging techniques suggest LSTV may be present in upwardly to 35.9% percent of the full general population.7
The germination of an LSTV may serve as a compensatory response to inadequate load bearing chapters of the sacrum13 or spinal instability secondary to weak iliolumbar ligaments.20 The resulting morphological alterations have important implications on spine surgery. Virtually incorrect level surgical procedures occur in patients with numeric variant spines or LSTV.12 Changes of neural arch elements and auricular surfaces complicate the placement of pedicle screws in an LSTV.14, 16 Lumbar interbody fusion at the junction above a fixed transitional level requires an alternative approach due to migration of neuronal anatomy within the psoas muscle and the more than caudal location of the junction between the common iliac veins and junior vena cava.27, 28
Spine physicians must identify the presence of LSTV prior to surgical intervention. The Ferguson radiograph serves equally the reference standard method to detect LSTV, though diagnostic errors and inaccurate identification of vertebral levels on both standard radiographs and MRI are common.43 The use of whole-spine images likewise every bit geometric relationships between the sacrum and lumbar vertebra assistance increment accuracy.5, 57, 58
Investigations regarding the association betwixt LSTV and clinically pregnant low back pain accept yielded inconsistent and conflicting results. Throughout the literature, Blazon 2 and Blazon IV are most consistently associated with back and buttock pain and decreased physical activity levels.9, 30 Symptoms associated with LSTV Blazon Ii potentially arise from degenerative changes in the pseudoarticulation between the transverse process and the pelvis.46 The germination of osteophytes in these "imitation joints" can cause nervus root compression.53 Disc herniation and degeneration virtually ever occur at the level supradjacent to the LSTV and may occur more frequently and at younger ages than in individuals without an LSTV.18, 20, 32
The pathophysiology of Bertolotti's syndrome remains obscure and in that location is no consensus most the most advisable therapy for each patient. Due to its multifactorial causes and the mutual findings of depression dorsum pain in the general population, information technology is essential to differentiate depression back pain caused by transverse mega-apophysis contact with the sacrum from other sources of back hurting in patients with LSTV.65 A positive radionuclide study along with a positive consequence from a local injection is almost helpful in establishing the diagnosis of a symptomatic pseudoarticulation. Meanwhile, selective radiculography serves as a reliable modality to diagnose far-out entrapment of the L5 nerve root. CT in combination with radiculography helps identify the point of impingement and the etiology of the L5 nerve root compression.80
The literature contains a total of 43 cases of surgical intervention for symptomatic LSTV. 27 patients were treated with resection, viii underwent fusion, 6 patients were treated for far-out syndrome, and the remaining ii cases involved surgical intervention for extraforaminal nervus root impingement or pain contralateral to the LSTV.47, 50–52, 63, 77–81 Merely Santavirta et al. compared the surgically treated patients to a bourgeois treatment control group. The results of surgical treatment were simply slightly better. The authors of these cases advocated for operative treatment of Bertolotti's syndrome in very select patients whose refractory pain is definitively attributed to the transitional vertebrae.78 Given the paucity of prove, farther investigations with larger patient cohorts are needed to meliorate understand the association between the anomalous transverse process and low back pain that occurs with LSTV and to ameliorate demonstrate the effectiveness of surgical intervention.64
Disclosures
The authors declare no relevant financial disclosures.
- Copyright © 2015 ISASS - This manuscript is generously published gratuitous of charge past ISASS, the International Social club for the Advancement of Spine Surgery
Source: https://www.ijssurgery.com/content/9/42
0 Response to "Partial Sacralization Left L5 Segment Is Again Appreciate"
Post a Comment